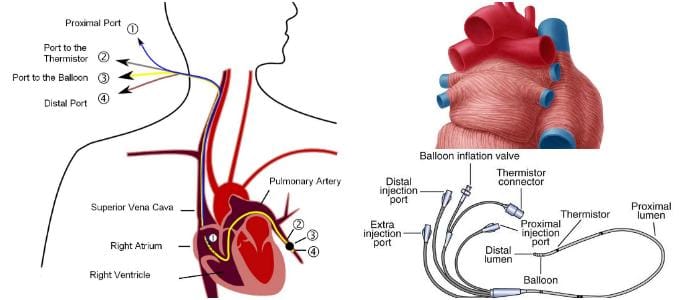
Pulmonary Wedge Pressure refers to the pressure within the pulmonary arterial system.
Many other terms exist to refer to Pulmonary Capillary Wedge Pressure (PCWP).
Some of them are Pulmonary Arterial Wedge Pressure (PAWP), Pulmonary Artery Occlusion Pressure (PAOP), or merely Pulmonary Wedge Pressure (PWP).
What is it?
PCWP is the left atrial pressure measurement obtained by the passing of a catheter from the right side of the heart into the pulmonary artery, wedging it into a small pulmonary arterial branch.
Even though medical experts can directly measure left the ventricular pressure by placing a catheter into the left ventricle, it won’t be very likely they can move this catheter back into the left atrium.
They may be able to measure left atrial pressure by placing a special catheter into the right atrium then punching through the interatrial septum.
However, medical experts usually don’t perform this technique because it brings some remarkable risks for their patients.
How doctors measure it?
Healthcare providers may measure PCWP by using a procedure called “Swan-Ganz catheter.”
The Swan-Ganz catheter is a type of pulmonary artery catheterization that usually consists of inserting a soft catheter into the pulmonary artery.
When it comes to measuring PCWP, doctors wedge a balloon-tipped, multi-lumen catheter into a peripheral vein such as the jugular or femoral vein.
The catheter has a lumen or a port that gets connected to a pressure transducer.
Doctors can determine the location of the catheter by taking a look at the pressure measured from the tip of the catheter.
In the right atrium (one of the upper chambers of the heart) the pressure average pressure is right below 5mmHg, fluctuating a few mmHg.
When the catheter enters into the right ventricle of the heart, the systolic pressure increases to approximately 25 mmHg.
While such rising occurs, the diastolic pressure remains similar to right atrial diastolic pressure.
When doctors get the catheter to reach the pulmonary artery, the systolic pressure is usually similar to the right ventricular systolic pressure.
However, the diastolic pressure rises to approximately 10mmHg because of pulmonic valve closure at the beginning of diastole.
The small balloon behind the tip of the catheter can get inflated with air.
When an expert accurately positions this medical device in a branch of the pulmonary artery, the distal port measures the pulmonary artery pressure of a patient.
The balloon gets inflated, which causes the occlusion of the pulmonary artery branch.
When that happens, the pressure in the distal port rapidly falls. But after waiting a few seconds, it reaches a stable lower value that is very similar to left atrial pressure.
The value recorded during balloon inflation is similar to the left atrial pressure of the patient because the occluded vessel and its branches act as an extension of the catheter that measures the blood pressures within the pulmonary veins and left atrium.
Why is it useful?
Measuring PCWP helps medical experts to diagnose conditions and diseases that may induce heart failures, which means the inability of the heart to supply adequate blood flow and oxygen to body and organs.
In this same regard, it can help to determine the severity of left ventricular failure and to quantify the degree of mitral valve stenosis.
Left ventricular heart failure can lead patients to develop pulmonary hypertension and right ventricular dysfunction.
Mitral Valve Stenosis consists of a narrowing of the opened mitral valve orifice, which makes it more difficult for blood to flow inside the heart.
Both of these conditions usually elevate left atrial pressure and PCWP.
Other conditions such as Aortic Valve Stenosis (which reduces the flow of blood), and Mitral Valve Regurgitation (which causes blood to flow back and engorge the atrium) also elevate left atrial pressure.
When these pressures are above 20 mmHg, the patient will likely develop Pulmonary Edema, a life-threatening condition.
By measuring PCWP, medical experts can titrate the dose of diuretic drugs and other medication that people tend to use to reduce pulmonary venous and capillary pressure.
Such medicines can prevent and, in several cases, reduce Pulmonary Edema. That makes the measurement PCWP a helpful mean to ensure or improve therapeutic efficacy.
It is essential to measure PCWP when evaluating Pulmonary Hypertension. The usual cause of this condition is, more often than not, increased pulmonary vascular resistance.
Doctors can use PCWP measurement to calculate it, along with some other techniques and procedures.
In some cases, Pulmonary Hypertension manifests as a result of increased pulmonary blood volume caused by left ventricular failure or some similar heart conditions.