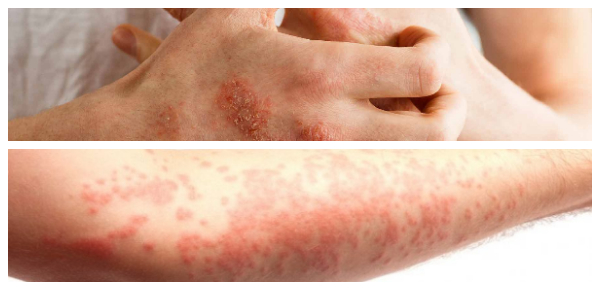
Eczema is a skin disease that produces inflammation, rashes, and blisters. It usually affects children, but sometimes adults can suffer from this condition as well.
Causes
Although eczema is more common in children, sometimes the disease affects adults who had not previously suffered from it.
Atopic dermatitis is not just a pediatric dermatosis. Although it usually begins almost always during infancy, and often before the age of two, it does not disappear in all cases before adolescence and adulthood.
It is estimated that around 10% of patients continue to suffer from eczema manifestations during adulthood. In some cases, this eczema remains a concern and may pose serious problems.
Adult atopic dermatitis is usually a severe dermatosis. These are chronic eczema plaques, red, thick and lichenified, sometimes accompanied by isolated prurigo papules.
In this context of chronic eczema, acute, vesiculous or exudative outbreaks occur.
Pruritus is always intense and influences the patient’s daily life, mood, sleep, and activities.
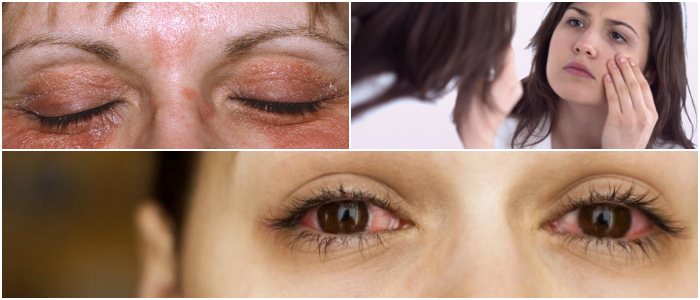
Its location is different from that of infantile atopic dermatitis. The hands, the face and especially the eyelids are often the most affected, as well as the large folds, although sometimes other areas of the body may also be affected.
Inflammatory outbreaks can impact the entire skin. In that case, we’re talking about erythroderma.
These generalized seizures are severe and can be complicated by infections and metabolic disorders, requiring hospitalization.
Atopic eczema (atopic dermatitis) is the most common form of inflammation. The causes of the disease are unknown.
However, there is a genetic component to the disease, since it tends to run in families. Allergens, such as dust mites, may set off an attack.
The disease tends to be aggravated by cold conditions, rough clothing, overuse of soaps, and stress. Foods are less likely to trigger attacks in adults than in children.
Contact eczema (contact dermatitis) is caused by contact with various substances, such as nickel, poison ivy, and some detergent ingredients.
Discoid eczema typically affects adults, particularly those with dry skins.
Are you sure it’s atopic dermatitis?
In the case of eczema in an adult, it is questionable whether it is atopic dermatitis, another type of disease or even an eczema-like dermatosis.
If the disease comes from childhood, it is accompanied by atopic respiratory manifestations, or even digestive allergies, and is a typical case clinically, in the form of thick chronic eczema, lichenified and sometimes with exudative outbreaks, can be sure of the diagnosis.
But if its appearance is recent and the clinical signs are not typical, it is possible to be faced with another dermatosis (contact eczema, scabies or lymphoma, among other types).
A skin biopsy may be performed to confirm eczema as well as control IgE levels or perform contact tests to rule out allergic contact eczema, which will be discussed later.
Symptoms
In atopic eczema, the skin becomes reddish and cracked. This condition tends to occur in folds of the flesh, such as between the fingers, in the elbows, under the knees, or around the ears and eyes.
Large areas of the skin are sometimes affected. Contact eczema typically affects the hands, giving red, itchy, and scaly skin. Discoid eczema takes the form of itchy, circular or oval patches of eczema.
Treatments
Emollient Creams (Moisturizing Creams) are the standard treatment for eczema. They need to be applied after washing.
The creams are usually designed to lock in the water behind a protective layer of oil, so preventing the skin from drying out.
Often the creams are based on paraffin wax or coconut oil. A recent study suggested that coconut oil was more effective than mineral oil for the treatment of atopic eczema.
Some emollient creams contain substances such as propylene glycol that absorb water.
Steroid Creams are often used to treat eczema. Hydrocortisone is a mild steroid treatment.
More powerful steroids include flurandrenolide (fludroxycortide, Cordran), betamethasone (Diprolene, Betnovate), and fluocinonide (Fluonex). Steroid treatment is often very effective when first used. However, eczema usually comes back.
Long-term treatment may lead to side-effects, such as thinning of the skin and eye diseases. Steroids creams should not be used near the eyes.
Oral Steroids, such as prednisone (Sterapred), are sometimes used in serious cases of eczema.
They have many side-effects, including osteoporosis, nausea, weight gain, high blood pressure, and risk of eye diseases, so should not be taken long-term.
Calcineurin Inhibitors, such as pimecrolimus (Elidel) and tacrolimus (Protopic), are sometimes used to treat eczema.
They are useful when steroid treatments can’t be used or are starting to give side-effects.
They sometimes give a burning sensation when first used. Some controversy exists as to whether or not they slightly increase the risk of some cancers.
Antihistamines are sometimes given to Eczema sufferers. They don’t heal eczema but can decrease the itchiness and help a sufferer sleep at night. Hempseed oil can be taken orally to lessen the symptoms of the disease.
A scientific study has shown that it was able to reduce the symptoms. The condition of patients consuming hempseed oil was compared to the status of a group taking olive oil.
The study was single-blinded, not double-blinded (the researchers knew which group of patients was having which treatment), so was not as perfect as it could have been.
Oatmeal Baths are a traditional remedy for eczema. Finely-powdered oatmeal (colloidal oatmeal) should be used.
A recent scientific review has concluded that oatmeal baths have a positive effect on atopic dermatitis in both adults and children.
The primary causes of allergic contact eczema are:
- Nickel contained in the metals of fantasy jewelry, glasses legs, and mobile phones.
- Preservatives in wipes, cosmetics and hygiene products (in particular, isothiazolinones).
- Rarely, other components of cosmetics such as perfumes or some sunscreens.
- The essential oils of some cosmetics known as “bio,” which offer no guarantee of hypoallergenicity at all.
- Rarely, certain clothing.
- The shoes (leather chrome, glue).
- Dermocorticoids themselves can become allergic, a particularly misleading allergy.
When there is suspicion of a contact allergy, it is advisable to perform the patch tests or epicutaneous. A positive patch test safely identifies the person responsible for allergic contact eczema.
But a simple interrogation and a measure of eviction, followed, if necessary, by a reintroduction, can also give very good results.