Endometrial biopsy is a procedure in which some tissue from the uterus.
During this test, a piece of the lining of the womb, known as endometrial tissue, gets removed for laboratory examination.
The procedure is necessary to detect diseases such as cancer of the womb lining (endometrial cancer) and endometrial hyperplasia (a non-cancerous over-proliferation of endometrial cells).
An endometrial biopsy is the removal of a small piece of tissue from the lining of the uterus (endometrium) to examine it.
Symptoms that indicate Endometrial Biopsy
A physician would typically recommend an endometrial biopsy when a patient displays signs that may indicate a disease of the endometrium (womb lining).
Symptoms such as unusual vaginal bleeding, particularly after the menopause, or between periods in pre-menopausal women, are usually investigated with an endometrial biopsy.
Other examination procedures, such as looking at the inside of the womb with a hysteroscope, may be carried out at the same time.
Other conditions, such as polycystic ovarian syndrome, can massively increase the risk of endometrial cancer; so a physician may recommend a biopsy to take a sample from the patient.
Medical experts may also carry on with an endometrial biopsy as part of an investigation into infertility, so they can check if the womb lining is responding as it should to the changing hormone levels in the menstrual cycle.
Description of the Procedure for Endometrial Biopsy
An endometrial biopsy should never be carried out on a pregnant woman; to prevent this from happening, the patient must take a pregnancy test before the procedure.
Doctors may need to delay a biopsy if any infection is present in the vagina or womb since there is a risk that the procedure may spread it further.
The patient is often given a painkiller, such as ibuprofen or acetaminophen (paracetamol), to minimize any pain or discomfort during the procedure.
Usually, medical experts use a local anesthetic. In some rare cases, a biopsy may have to be taken using a general anesthetic (for example if the opening of the cervix is much more narrow than usual).
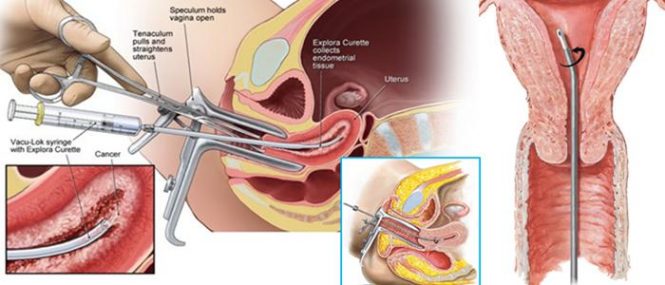
An instrument called speculum is inserted into the vagina to widen it to allow access to the cervix and womb.
A tool called a tenaculum (a type of forceps) is used to keep the cervix open, while a biopsy instrument (usually a curette) is used to collect a sample of endometrial tissue from inside the womb.
There may be some pain or vaginal bleeding after the procedure. However, it is vital that patients immediately contact a physician if symptoms persist or they acquire a fever.
Complications
An endometrial biopsy is quite a low-risk procedure. Some rare complications include perforation of the womb or bacterial infection.
However, nobody should feel deterred from having a biopsy out of fear for complications or any other reason. The alternative is to leave a severe disease untreated or to continue to worry for no good cause.
Results and Further Treatment
Laboratory analysis of the tissue sample can determine whether any abnormality is present.
The tissue examination can distinguish between endometrial hyperplasia (a non-cancerous over-proliferation of endometrial cells) and cancer of the uterus.
Appropriate treatment can then commence. If cancer is present, a hysterectomy is a standard procedure. Endometrial hyperplasia may respond to hormone treatment.
In the case of fertility problems, a physician can use the results to determine which further treatments are needed.
If the womb wall is responding to hormones in a usual way, the reason for infertility must lie elsewhere.
How the test is performed.
Physicians can perform this procedure with or without anesthesia (this is a medicine that allows you to sleep during the treatment).
You lie on your back with your feet resting on stirrups. Your healthcare provider gently inserts an instrument (speculum) into the vagina to keep it open, so that he can see the cervix.
The cervix gets cleaned with a special liquid and anesthesia can be applied. Then the cervix can be gently grasped with an instrument to keep the uterus still.
Doctors may need another instrument to gently stretch the cervical opening, in case there is rigidity.
An instrument is gently passed through the cervix into the uterus to collect the tissue sample. The doctor removes the tissue sample.
He sends the tissue to a laboratory. There, they examine it under a microscope. If you were given anesthesia for the procedure, then the nursing staff will take you to the recovery area.
They will make sure you are comfortable. After you wake up and have no problems following anesthesia and the procedure, you will be allowed to go home.
How the test feels.
Instruments can feel cold. You may feel some pain when you hold the cervix, as well as some cramping the moment the tools enter the uterus and when doctors take the sample.
Preparation for the exam.
Before the test:
- Tell your provider about all the medicines you take. These include anticoagulants such as warfarin, clopidogrel, and acetylsalicylic acid (aspirin).
- You may be asked to have a test to see if you are pregnant.
- Do not use creams or other medicines in the vagina from 2 days before the procedure.
- DO NOT use vaginal douches. (You should never use these showers as they can cause infections of the vagina or uterus).
- Ask your provider if you should take analgesics, such as ibuprofen or paracetamol, right before the procedure.
Reasons for the exam.
The test is done to find the cause of:
- Abnormal menstrual periods (profuse, prolonged or irregular bleeding)
- Bleeding after menopause
- Bleeding from taking hormone therapy medicines
- Thickening of the uterine lining observed on an ultrasound
- Endometrial cancer
Risks.
The risks of an endometrial biopsy are:
- Infection.
- Causing a hole (puncture) in the uterus or tearing the cervix (rarely occurs).
- Prolonged bleeding.
- Light spotting and mild cramping for a few days.
Normal values.
The biopsy’s results show nothing of concern if the cells in the sample are not abnormal. But what would abnormal results mean?
Irregular menstrual periods can be caused by:
- Uterine fibroids.
- Fingerlike masses in the uterus (uterine polyps).
- Infection.
- Hormonal imbalance.
- Precancer or endometrial cancer (hyperplasia).
Other conditions under which doctors may perform this test are:
- Abnormal bleeding if the woman is taking the breast cancer drug, tamoxifen.
- Abnormal bleeding due to changes in hormone levels (anovulatory bleeding).
